Tendon Disorders
On this page
What are tendons?
Back to topTendons are rope-like bundles or bands of strong, smooth, shiny fibres that attach muscles to bones. They transfer force from the muscle to the bone to produce the movement of joints. There are two types of tendons: tendons without sheaths (Figure 1), and tendons with sheaths (Figure 2).
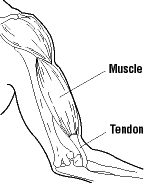
Figure 1
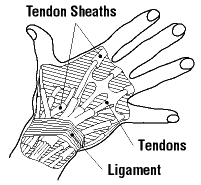
Figure 2
What are tendon disorders?
Back to topTendon disorders, or tendinopathies, are medical conditions that cause the tendons not to function normally. Tendinitis is a disorder of tendons without sheaths and tenosynovitis is a disorder of tendons with sheaths.
What is tendonitis?
Back to topTraditionally, tendinitis (also called tendonitis) is the term used to describe an inflammation or irritation of a tendon. With repetitive or prolonged activities, forceful exertion, awkward and static postures, vibration, and localized mechanical stress, the tendon fibres can tear apart in much the same way a rope becomes frayed.
These tendon changes trigger an inflammatory response. Inflammation is a localized response of tissue to injury. Over time, inflamed tendons become thickened, bumpy, and irregular. Without rest and time for the tissue to heal, tendons can become permanently weakened.
Tendinosis (also called tendonosis) is the preferred term to describe chronic pain associated with a symptomatic tendon.
What is tenosynovitis?
Back to topTenosynovitis is an inflammation of the tendon sheath. The tendons are protected by a membrane (synovial membrane) which lubricates the tendon. With repetitive or prolonged activities, forceful exertion, awkward and static posture, vibration, and localized mechanical stress, the lubrication system may malfunction. It may not produce enough fluid, or it may produce a fluid with poor lubricating qualities. These factors may lead to inflammation and swelling of the tendon sheath. Repeated episodes of inflammation cause fibrous tissue to form that thickens the tendon sheath and hinders tendon movement.
Where do tendon disorders occur?
Back to topThe most common sites for occupational tendon disorders are (Figure 3):
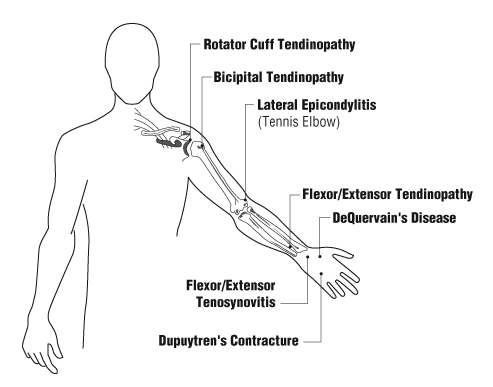
Figure 3
- Bicipital tendinopathy – a disorder of the tendon to the biceps.
- Rotator cuff tendinopathy – disorder of the tendons that rotate the humerus (upper arm bone) and help raise the arm.
Lateral epicondylitis or tennis elbow – tendon inflammation that attaches some forearm muscles to a "bump" or projection (lateral epicondyle) on the side of the humerus, just above the elbow.
- Flexor tendinopathy – a disorder of the tendons in the palm side of the wrist and hand.
- Extensor tendinopathy – a disorder of the tendons in the back of the hand and wrist (or other body parts, such as the feet).
- Flexor tenosynovitis – inflammation of the tendon sheaths in the palm side of the wrist and hand.
- Extensor tenosynovitis – inflammation of the tendons in the back of the hand and wrist.
- De Quervain's disease – inflammation of the tendon sheaths at the base of the thumb.
Shoulder tendinopathy
The most common tendon disorders of the shoulder are bicipital tendinopathy and rotator cuff tendinopathy. Bicipital tendinopathy may be caused by inflammation of the tendon around the biceps muscle, or by degeneration of the tendon from repetitive overhead motion or the normal aging process. Rotator cuff tendinopathy is also known as supraspinatus tendinitis or partial tear of the rotator cuff. Many people with shoulder tendonitis also have shoulder bursitis (swelling of the bursa).
Tendon disorders of the shoulder are seen among workers exposed to highly repetitive movements requiring significant use of force. Workers doing jobs requiring awkward postures such as overhead work, arm elevation, and specific postures relative to the degree of arm bending and arm elevation.
Elbow tendinopathy
Tendinopathy of the elbow, also known as tennis elbow or lateral epicondylitis, is associated with jobs that require repeated or forceful movements of the fingers, wrist, and forearm. Specific movements associated with developing tendinopathy of the elbow include simultaneous rotation of the forearm and bending of the wrist, stressful gripping of objects with inward or outward movement of the forearm, or jerky throwing motions. For more information, please refer to our OSH Answers document on Tennis Elbow.
Hand and wrist tendinopathy
Tendinopathy of the hand and wrist includes a variety of diagnoses, such as tenosynovitis, tendinitis, and De Quervain's disease.
High-risk occupations and activities associated with hand and wrist tendinitis include assembly line work, meat processing, manufacturing, knitting, typing, and piano playing.
There is some evidence that workers exposed to risk factors such as high force and high repetition are at increased risk for hand and wrist tendinopathy. Excessive texting on cellular phones has been found to be a potential risk factor.
Patellar (knee) tendinitis
Patellar tendinitis is an injury to the tendon connecting your kneecap (patella) to your shinbone. This tendon helps to extend your knee so you can kick, run, and jump. Running and jumping are the most common causes, but sudden increases in how hard or how often you run or jump can add stress. While common in athletes, people in occupations with similar movements may be at risk.
What are the symptoms?
Back to topThe clinical presentation of tendon disorders is characterized by pain at the injury site. Often, there is also a decrease in strength or functional ability. Specific physical findings on examination include tenderness when the area over the affected tendon is touched, which may be associated with swelling, redness, and restriction of movement.
What causes tendon disorders?
Back to topOften, it is a combination of factors that leads to a tendon disorder, and every situation is unique. Causes can include overuse as well as age, injury, or disease-related changes in the tendon. Risk factors for tendon disorders can include excessive force, repetitive movements, frequent overhead reaching, vibration, and awkward postures.
What are treatment options?
Back to topTreatment of tendon disorders is of a conservative nature and rarely requires surgery.
Avoiding those activities that caused or aggravated the disorder will prevent the condition from persisting or recurring. Pain relievers, corticosteroids, dry needling, or platelet-rich plasma may be options to discuss with your medical professional. Physical therapy can help stretch and strengthen the affected muscles and tendons.
How can we prevent tendon disorders?
Back to topTendon disorders have been associated with repetitive or prolonged activities, forceful exertion, awkward and static posture, vibration, and localized mechanical stress. The prevention of tendon disorders should include identifying and remedying these risk factors.
Good design of work practices and equipment should reduce repetitive movements, awkward postures and static posture (periods spent in one position). Job design should also aim at minimizing the need to use forceful exertion and making sure that rest and work breaks are properly used.
The prevention of tendon disorders should also include training and education. To be successful, a training and education program must be organized, consistent, and ongoing. Everyone at work, including workers, managers, health and safety representatives, etc., must get actively involved. Education and training can include:
- The proper techniques for each task (e.g., appropriate lifting techniques).
- Work organization and policies (e.g., job rotation, rest breaks, allowing time to stretch at the beginning of the shift)
- How to use the available tools and equipment correctly.
- Good ergonomic setup.
- Fact sheet last revised: 2024-04-23

