Business Continuity Plan - Pandemic
On this page
- What is a business continuity plan?
- Is a pandemic plan different than a regular business continuity or resumption plan?
- How many people will be away from the workplace during a pandemic?
- What are some effects of a pandemic on a business?
- How do you set priorities for your plan?
- What are elements that should be included in a business continuity plan for pandemics?
- Using an office setting as an example, how can the office space accommodate physical distancing requirements?
- What are other good practices to help reduce the spread of infectious diseases?
- What should we be aware of for COVID-19 symptoms?
What is a business continuity plan?
Back to topA business continuity plan is a document that outlines how an organization will continue to function during and after an emergency or event. It involves planning how your key services or products can continue.
Please remember... each business is unique – the topics listed in this document are general suggestions. You will need to create a specific plan that best suits your business and operational needs.
This document focuses on creating a business plan for infectious diseases such as a pandemic or severe seasonal outbreak that results from a virus or other agent. It is intended for non-healthcare organizations. Healthcare organizations, as well as other first response agencies (e.g., police, emergency, first aid, ambulance), will require more rigorous infection control measures and workforce plans.
Please see the OSH Answers "Emergency Planning" for information on a general emergency response plan.
Is a pandemic plan different than a regular business continuity or resumption plan?
Back to topIn some ways, yes.
Traditionally, most business continuity plans focus on what will happen if the building or equipment is damaged. In other scenarios, the plan may assume that people will be able to return to a building after a single event (such as after a storm or if there is a utility outage).
However, if there is a serious infectious disease outbreak, such as a pandemic, you must plan for the workers to be unable to report to work for a period of time. During a pandemic, businesses, social organizations, or schools may be required to close by order of health officials to help slow the spread of the illness. These steps will influence how many people may be available to report to work. Other measures may be enacted by governments or recommended by public health officials, such as physical distancing, hand hygiene, travel restrictions, limits to the number of people who can gather at a single location, alternative, use of non-medical masks, etc.
It is important to plan to have your core business activities remain operational for several weeks or months with limited staff like working remotely.
Please see the booklet Business Continuity Plan: Infectious Diseases for more information.
How many people will be away from the workplace during a pandemic?
Back to topIt is hard to say with certainty. Every pandemic is different. It will depend on the virus's “viral ability” – that is, how easily the virus spreads and how sick people become. Workers may be away from work for various reasons (e.g., illness, caregiving, school closure).
Also note, as stated by the Government of Canada: “The pattern of disease is different in pandemics than in seasonal influenza. Pandemics may arrive outside of the usual influenza season and typically have more than one wave of illness. The total duration of a pandemic is likely to be 12 to 18 months.”
It will be important to make sure your plan will accommodate staff absences for more than a single period of time.
What are some effects of a pandemic on a business?
Back to topPossible effects on business from a pandemic can include:
- reduced labour supply, including your regular workers or availability of contractors or temporary workers
- reduced business or cancelled customer orders
- interruption in getting supplies or materials (especially if goods are imported by air or land)
- change in demands (for example, increased internet use, decreased tourism/travel, alternative methods to conduct business such as curbside pick up or delivery)
- reductions or restrictions on public meetings or gatherings (including schools, sports, clubs, theatre, community centres, restaurants, religious gatherings, etc.)
- restrictions on travel (regional, national, or international)
- reduced availability of health care or home care services
- reduced availability of child day care services
- in more severe situations, disruptions in services such as telecommunications, financial/banking, water, electricity, gasoline/fuels, medicine, or the food supply
How do you set priorities for your plan?
Back to topIn general, when creating a business continuity plan, determine what element is critical and how the loss of this element will affect the business.
- Identify critical processes, operations, and functions.
- Identify key internal and external dependencies – those things, people, or other businesses you rely on.
- Identify what else can affect your business.
When planning for your priorities, examine:
- Personnel – Identify and train backups for essential functions, including chain of command (management). Be sure you have consulted with staff, including any applicable union or collective agreements.
- Equipment – Make sure the available equipment meets the identified needs.
- Availability of assets – Make sure that facilities, utilities, computers, machinery, or tools also meet your needs (e.g., access to internal systems by staff working from home).
- Business commitments – Research legal implications for the level of service arrangements (e.g., for non-performance or late delivery).
- Accounting – make sure you can continue your payroll, finances, etc.
Elements of a risk assessment process may also be helpful.
What are elements that should be included in a business continuity plan for pandemics?
Back to topHow detailed your plan is will depend on the type of business, how complex your organization is, and its size. Allow your plan to be flexible and proportional to match the level of threat that is occurring at that time. As a pandemic evolves, restrictions may be lifted or tightened, as determined by local public health officials. It may also be the case that certain geographical areas have different levels of measures in place. Your plan should include health, safety, human resources, and management elements.
Options include:
- Document guidelines for management and business decisions – remember, anyone can get sick.
- Create a pandemic management team that assigns who will do what tasks, establishes a chain of command, coordinates prevention activities, etc.
- Make decisions about when to stay open, when to close to customers, when to use alternative methods to conduct business, and when to close completely.
- Assign a person or team, where appropriate, to help assess the health of workers (e.g., if the worker may be coming down with an illness) such as by using screening checklists as provided by public health officials.
- Cross-train workers to make sure essential functions will continue (e.g., payroll, customer service).
- Provide handwashing facilities and/or alcohol-based hand sanitizers (of at least 60% alcohol).
- Have a period of time between shifts to clean touch points and surfaces such as tables, door knobs, handrails, shared telephones and keyboards.
- Have up-to-date sick leave policies. NOTE: Be aware that doctors may have limited availability to provide sick leave documentation.
- Maintain an up-to-date list of your staff and your clients (e.g., telephone trees, call-in numbers, hot lines for information, broadcast e-mails)
- Develop communication methods to reach all staff, especially if staff are working remotely.
- Develop methods to conduct your business, including using the internet, cloud-based workspaces, phones, video conferencing, etc.
- Develop methods that allow workers to use flexible work options or telework/work remotely.
- Increase the distance between people (e.g., install a protective barrier for those working with the public, increase the distance between workstations, use larger meeting rooms, limit the number of users in a common area such as a lunch room or washroom).
- Consider providing transportation for those staff who use public transportation.
- Consider psychosocial issues (e.g., financial stress, caregiver burnout, occupational stresses, stigma, or social exclusion).
- Consider postponing or cancelling face-to-face meetings (including internally) as well as unnecessary travel.
- Create small working groups or "cohorts" (e.g., a factory may keep the same group of people together on the same shifts).
- Document which workers were present each day to assist public health with contract tracing if a case is discovered.
Using an office setting as an example, how can the office space accommodate physical distancing requirements?
Back to topThere are three key areas to consider:
- the space and equipment an individual uses
- the common use spaces, such as meeting areas, social areas, lunch rooms, and equipment rooms, as well as the paths of travel
- personal measures, such as hand hygiene and respiratory etiquette
The workplace should evaluate who needs to be in the office and how they will function in the space. It may not be possible to allow your normal capacity of people in the building and maintain physical distancing at the same time. Additional factors include “congestion points” such as kitchens, lockers, closets, elevators, stairs, washrooms, and emergency exits.
Public Services and Procurement Canada (2020) have developed a "Guidance and practices for the safe return to workplaces in light of the easing restrictions" document. When assessing the workstation layout, be sure to measure for 2 metres distance in all directions, measured from where the individual would sit.
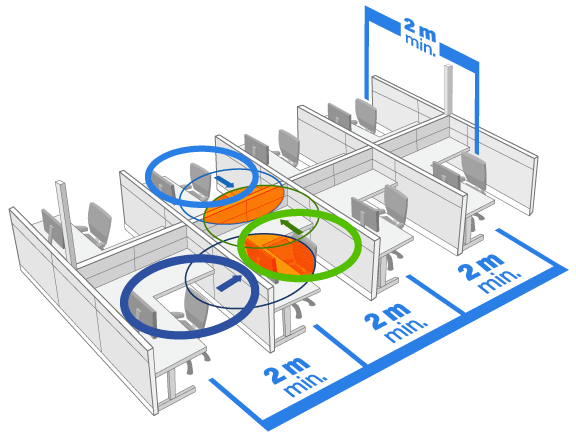
Public Services and Procurement Canada note that "there is no evidence that partitions provide sufficient safety between occupants, and should not be the first line of defence". Maintaining 2 metres physical distance is preferred. When considering additional partitions or other barriers, also determine if the installation will reduce the effectiveness of the ventilation systems.
Staggered seating or re-arrangement of desks may help. Face-to-face seating is discouraged.
Other measures may include:
- making sure the ventilation system is working appropriately. Increase air refreshment rates, if possible.
- allowing workers to work at the same desk each day if seating arrangements would normally be flexible
- asking workers to maintain a tidy desk to assist with cleaning and disinfecting
- removing extra chairs from meeting rooms to help avoid overcrowding
- using wide tables when individuals are sitting face-to-face
- keeping doors open to assist with air circulation
- indicating a path of travel in hallways, especially if the hall will not allow persons to pass and maintain physical distancing
- labelling doors as entry or exit only
- allowing only 1 person in an equipment room or kitchen at a time
- if allowing the use of microwaves, fridges, etc, in the office, providing a method to clean the surfaces after use
- waiting until the other person has left before approaching a locker or coat closet
- marking spots outside meeting rooms or washrooms where people should wait before entering
- allowing time between meetings to allow for the air in the room to refresh
What are other good practices to help reduce the spread of infectious diseases?
Back to topGood health habits are important in preventing the spread of infectious diseases. Steps to take include:
- keeping up to date with vaccinations
- staying home when sick, even with mild symptoms
- frequent hand washing with soap and water
- using alcohol-based hand sanitizers (at least 60% alcohol) when soap and water are not available
- avoiding close contact with sick people
- coughing and sneezing into your elbow, or use a tissue (and throw away the tissue immediately)
- avoiding touching your eyes, nose and mouth
- using proper hygiene practices, such as cleaning and disinfecting surfaces likely to be contaminated and touched by others
What should we be aware of for COVID-19 symptoms?
Back to topWhen a person is infected with COVID-19, they may have little or no symptoms, and the symptoms they do show can be easily confused with a cold or seasonal flu.
COVID-19 appears to mainly spread from person to person when people are in close contact with one another (within about 2 metres or 6 feet) and through respiratory droplets produced when a person coughs or sneezes. These droplets can land in the mouths or noses of people who are nearby or possibly be inhaled into the lungs.
It is possible that it can spread from contact with infected surfaces or objects – when you touch a surface or object that has the virus on it and then touch their own mouth, nose, or eyes.
Note that the Government of Canada states that there is evidence which indicates that the virus can be transmitted to others from someone who is infected but not showing symptoms. This transmission includes people who:
- have not yet developed symptoms (known as pre-symptomatic)
- never develop symptoms (known as asymptomatic)
Cold | Seasonal Influenza | COVID-19 |
|---|---|---|
| Chills but fever is rare | Fever | Feeling feverish |
| Cough, chest discomfort (mild but may last a while) | Cough, chest discomfort (dry cough can be severe) | Cough (new or worsening) |
| Body aches, pains (mild) | Body aches, pains (can be severe) | Difficulty breathing or shortness of breath |
| Tiredness (you can still do your daily activities) | Bedridden (you may feel extremely exhausted) | Chills |
| Headache (mild) | Headache (can be severe) | Fatigue or weakness |
| Sore throat | Sore throat | Muscle or body aches |
| Stuffy, runny nose, sneezing | Stuffy, runny nose | New loss of smell or taste Other symptoms include: |
| Complications can include… | ||
| Lung infections Throat infections Ear infections Sinus infections | Pneumonia Pre-existing health conditions getting worse (such as asthma) Hospitalization Death | Pneumonia in both lungs and death |
Table adapted from: Cold or flu: know the difference / Know the flu facts - Fact sheet, Government of Canada, 2019, and COVID-19: Symptoms, treatment, what to do if you feel sick, Government of Canada, 2020.
- Fact sheet last revised: 2024-03-20

